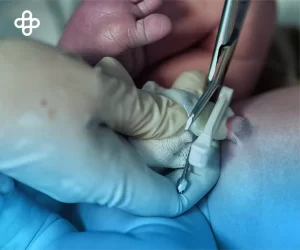
Diabetic foot is a condition characterized by infection, ulceration, and/or tissue destruction in the foot. It is typically associated with diabetic neuropathy (nerve damage in the foot) or peripheral arterial disease (damage to the arteries that supply blood to the foot) and is usually located below the ankle.
This definition has been established by the World Health Organization (WHO). The International Working Group on the Diabetic Foot (IWGDF). And the Latin American System of San Elian of the Latin American Diabetic Foot Association (ALAPID).
“If a diabetic patient notices an ulcer on their foot, they should immediately consult a specialist. Both to treat it as soon as possible and to discover the cause of its origin. Which will allow us to design a personalized treatment suitable for their case.”
- Dr. Javier Escalada San Martín, University of Navarra
Amputations
Diabetic foot is a complication of Diabetes Mellitus that can lead to limb amputation. In fact, 90% of amputations begin with a small, painless foot lesion due to decreased sensitivity. Patients often seek medical attention after their condition has worsened. Did you know that we can prevent up to 85% of amputations? Yes, contact your doctor immediately.
Diabetic foot has a negative impact on the quality of life of affected individuals. It is one of the leading causes of hospitalization in people with diabetes and presents a challenge for healthcare professionals. It is a complex problem to address due to the numerous procedures patients must undergo and the high costs associated with its treatment.
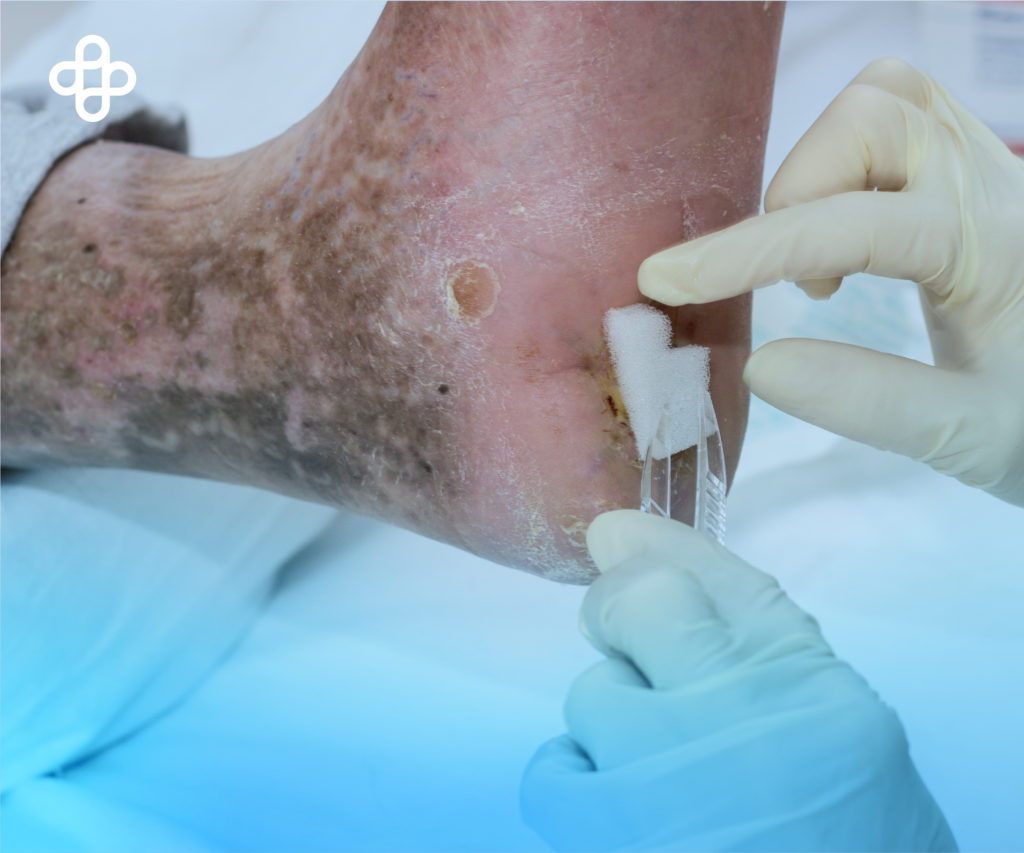
The feet of people with diabetes are prone to various types of injuries. For this reason, it is important for those with diabetes to perform a daily examination. It is essential for them to educate themselves about wound care and proper cleaning techniques to prevent infection and identify new wounds in a timely manner. However, it’s important to consult with a doctor as soon as possible for treatment once you’ve identified a wound.
The Wagner Classification of Diabetic Foot
In 1970, Dr. Wagner developed a classification system to set standard criteria for diagnosing and treating diabetic foot issues. This classification is the most commonly used for assessing diabetic foot injuries.
The Wagner Classification is as follows:
- Grade 0: Patients with no ulcers but at high risk.
- Grade 1: Superficial ulcer affecting only the skin’s full thickness, not involving underlying tissues.
- Grade 2: Deep ulcer, penetrating ligaments, and muscles but not involving bone or abscess formation.
- Grade 3: Deep ulcer with abscess formation and bone involvement.
- Grade 4: Localized gangrene.
- Grade 5: Extensive or diffuse gangrene involving the entire foot.
Stem Cells and Diabetic Foot
The treatment of diabetic foot with adult stem cells is yielding excellent results in various studies worldwide.
Moreover, The treatment involves the extraction of stem cells from the patient’s own fat tissue. After processing and activating them using a high-tech protocol and system, healthcare professionals administer these stem cells intravenously. This allows the stem cells to reach areas of the body with inflammation and low oxygen levels. Particularly, for diabetic individuals, these cells primarily target the pancreas.

Similarly, you can apply these stem cells locally to the ulcerated areas when there are lesions on the lower limbs. Additionally, their primary purpose is to enhance their action at the sites of greatest damage. Indeed, the key benefit of applying stem cells is their ability to generate new blood vessels, which improves the oxygenation of the lesion, enhances the healing process, and reduces the risk of infections.
Finally, to stay updated on the latest research on this condition and stem cells, I invite you to read our article “Stem Cells and Diabetic Foot.“